Author: Dave Marshall-George, Sales Director, Condair Ltd
Making buildings healthier
Every winter we suffer a rise in colds, flu and respiratory illnesses. It seems as inevitable as an increase in pollen allergies in the spring or sunburn in the summer.
The main reasons put forward for this seasonality of illness are that people spend more time together indoors, cold dry air weakens our immune system and it offers a more hospitable environment for viruses to thrive in. These factors combine to create a situation where respiratory viruses spread more easily from person to person, resulting in increased infection.
But, does it need to be this way? Could we better manage our indoor environments to counter these factors, curb the rise of seasonal illness and provide a return on the investment through increased productivity and reduced healthcare costs? I think the answer is yes, yes and yes!
The SARS-CoV-2 pandemic has focused public attention on how viruses are transmitted. Public awareness has already come a long way from washing hands whilst singing happy birthday, to understanding more about how a room’s CO2 concentrations provide an indication of adequate ventilation in a building.
This awareness is here to stay, even beyond a vaccination program that will hopefully wipe COVID-19 off the face of the earth. And this awareness will grow. Informed building occupants are going to be demanding much more from a building operator or employer than the correct temperature, adequate lighting and a comfy chair. The need for improved ventilation has taken centre stage recently in media coverage, but awareness of other factors, such as the impact of indoor humidity on our health, is also increasing.
In their recommendations on how to operate buildings safely, CIBSE and ASHRAE have prominently endorsed 40-60%RH as the ideal humidity level to mitigate viral transmission. The European Centre for Disease Prevention and Control also recently recommended this level in its HVAC guidance, as have authoritative international bodies, such as Germany’s FGK and Australia’s AIRAH.
In the recent online BESA Conference, Dr Taylor, of ASHRAE’s Epidemic Task Force, gave a thorough presentation on the science behind why 40-60%RH is the optimum indoor humidity for respiratory infection control. The ASHRAE Distinguished Lecturer said numerous studies had identified an RH “sweet spot” of between 40% and 60%, because “there are fewer virus particles in the air, they are less infectious and our health and immunity is much better, when we have our humidity in this zone.”
Dr Taylor also presented a study she recently undertook in association with the MIT research university in the US. COVID-19 infection and death rates were examined in 125 different countries alongside a huge variety of other variables and examined for correlations. The study found that when the indoor relative humidity was low, the COVID-19 infection rates were higher. Conversely, when the indoor humidity was midrange, death rates were at their lowest.
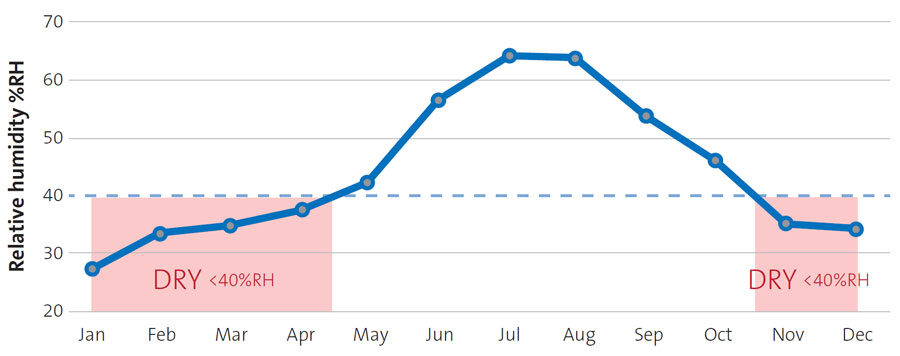
In the UK, we can expect to experience an indoor humidity below this “sweet spot” of 40-60%, when the outside temperature is around 8°C and the indoor environment is heated to 20°C or more. This will typically happen from around November through to March. This indoor dry season corresponds perfectly to the rise and fall of seasonal winter respiratory illnesses in the UK.
Although the science demonstrating the benefits of maintaining 40-60%RH is comprehensive, as we have no sensory perception of air humidity, public awareness of what humidity is and its impact on us has been very limited. We can’t feel whether our rooms are dry or humid, unless it’s at the extreme. We therefore do not commonly associate experiencing consistently dry environments with any subsequent ill health.
Even with public awareness now growing of the benefits of a midrange humidity, many people are unaware that humidity control in buildings even exists. In many recent mainstream media articles, even though 40-60%RH is accepted as an ideal level, when humidification is suggested as a protective measure, it’s frequently dismissed as being somehow unachievable or an impractical solution. This definitely is not the case and demonstrates a lack of awareness about the role commercial humidification currently plays in our built environment.
We routinely humidify factories, data centres, museums, storage facilities and a whole host of other buildings, big and small, when a manufacturing or process application requires it. Humidification of offices for health is reasonably commonplace among informed building operators. Humidification of hospital environments is also routine, but is limited to areas where humidity control is deemed necessary for the particular application, such as in MRI suites. The return on investment in performing more accurate scans is evident but the return on investment in humidifying wards and waiting rooms, to protect staff and patients from aerosol cross infection is, unfortunately, not so immediately perceivable.
Given that the health benefits of humidification are scientifically clear, but not immediately obvious to the occupants’ senses, I feel it will take government regulatory change to ensure optimum indoor humidity levels are maintained in public buildings. Otherwise, in the drive to minimise operating costs, humidification will frequently be omitted, along with other beneficial but concealed services.
In the battle to make our buildings healthier, there are many weapons in the building services’ arsenal. Humidity control is an important but individual factor, alongside other activities such as correct ventilation, air filtration, lighting and occupant density. Many of these protective strategies complement each other and when combined will significantly improve occupant health.
By upgrading our built environment in this way we will be protecting society, not just from the threat of potential future pandemics, but also by significantly reducing the many deaths, sick days, lost productivity and healthcare costs associated with winter seasonal illness.