
Humidity Fights Flu
An indoor humidity level of between 40-60%RH has been scientifically proven to combat airborne flu infections. This ideal humidity level shortens the time airborne flu remains infectious.
The scientific studies below are just a few of the many that show how the correct indoor humidity is vital for airborne infection control.
During the cold winter months, when heating systems dry the air, indoor humidity often drops into the dry danger zone of less than 40%RH. This results in more flu and respiratory infections spreading in the indoor air we all share.
Using humidifiers to put moisture into an atmosphere is only way to ensure the ideal indoor humidity is maintained throughout the winter.
40-60%RH is the ideal indoor air humidity. At this level, the airborne flu virus is quickly inactivated and air humidity is below the level that promotes mould growth.
Dr.med Walter Hugentobler

The science behind humidity's fight with flu
Noti et al 20131
Manikin experiment
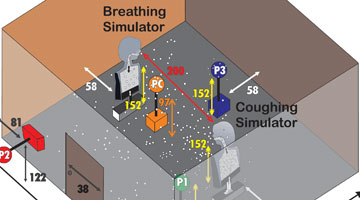
Method: Manikins “coughed” flu from nebulizers into a room at different humidity levels. Air samplers collected aerosol particles to assess their continued infectious nature.
Summary result: Flu retains its infectious nature in dry air below 40%RH up to five times longer than in air above 40%RH.
Yang et al 20122
Droplet observation
Method: Measured the survival of flu in droplets of different solutions at varying humidity levels to isolate the effects of humidity and the host droplet’s composition on flu.
Summary result: At room temperature, flu survival rate is lowest at around 50%RH, due to salt concentrations of the host droplet being most damaging to the virus at this level.
Lowen et al 20073
Guinea pig experiment
Method: Placed caged guinea pigs infected with flu next to uninfected caged guinea pigs, in a controlled environment at different humidity levels to assess humidity’s effect on transmission.
Summary result: Flu transmission between guinea pigs was lowest at 50%RH and significantly increased as the humidity decreased.
Absenteeism studies
Sale 19724
Nursery study

Method: Winter absenteeism from respiratory infections was recorded across two nurseries without humidification (ave. 35-40%RH) and compared to one nursery with humidification (ave. 50%RH).
Summary result: Child absenteeism from respiratory infections was 7.1% in the group without humidification and 1.3% in the group with humidification.
Gelperin 19735
Army study

Method: Incidents of respiratory infection in two groups of army recruits was monitored in two barracks; one with humidification (ave. 40%RH±5%) and one without humidification (ave. 20%RH±8%).
Summary result: Incidents of respiratory infections across two winters and 1,560 recruits was 14% lower in the humidified barracks than the non-humidified barracks.
Green 19816
Hospital study

Method: Staff absenteeism was monitored across three hospitals during subsequent winters. Two hospitals had no humidity control (ave. 19-22%RH) and one had humidification (ave. 31-34%RH).
Summary result: The average absenteeism rate in the non-humidified hospitals was 2.5%. In the humidified hospital this was reduced to 1.87% in one year and 1.56% the following year.

HEALTH PODCAST
Check out this podcast on how maintaining 40-60% relative humidity indoors is important in combatting the spread of viral infection.
You may also be interested in...

My humidity is low, what should I do?

Get a hygrometer

The science behind a healthy humidity

Return to work: how to manage a healthy humidity
References:
2 – Yang et al 2012, Relationship between Humidity and Influenza A Viability in Droplets and Implications for Influenza’s Seasonality, PLoS ONE 7(10): e46789
3 – Lowen et al, 2007, Influenza virus transmission is dependent on relative humidity and temperature, PLoS One Pathogens Okt. 2007/Vol. 3/Issue 10/e151
4 – Sale, 1972, Humidification to reduce respiratory illnesses in nursery school children, Southern Medical Journal, July 1972, Vol. 65, No 7
5 – Gelperin, 1973, Humidification and Upper Respiratory Infection Incidence, Heating, Piping and Air Conditioning, Vol. 45, No.3
6 – Green, 1981, Winter humidities and related absenteeism in Canadian hospitals, Digest of the 3rd CMBFS Canadian Clinical Engineering Conference
